

Although the minimum age requirement for becoming a doctor was 21 cheap furosemide 100 mg without prescription, this rule was not strictly followed order furosemide 40 mg otc. Instead of intensive laboratory and clin- ical preparation furosemide 40 mg mastercard, students learned solely by attending lectures buy furosemide 40 mg cheap. The medical schools of the era were proprietary schools; that is, the lec- turers who instructed the students often owned the schools. The face of medical education changed in the mid-nineteenth century as American doctors began to travel more extensively in Europe, where they were exposed to the new laboratory methods being developed by European doctors. At the same time, the mod- ern university was emerging, and new regulatory authority was being assumed by state and federal governments. By 1910, when Abraham Flexner published his famous report that outlined the 13 Copyright © 2005 by The McGraw-Hill Companies, Inc. With the growth of medical knowledge, research and teaching became full-time activities for some in the medical profession. By the late nineteenth century, the academic physician who taught medical students was prominent. In the twenty-first century, the division between academic and clinical medicine still exists. Preparing for Medical School Admission to medical school is extremely competitive. In 2003 there were about 35,000 applicants for the 16,538 available spots at the 125 medical schools in the United States. Thus, the chances of getting into medical school—any medical school—are less than 50 percent. Most applicants want to attend what they consider the “best” medical schools. Due to the strict accreditation requirements of the Liaison Committee on Medical Education, medical schools do not vary widely in educational quality. But many factors influence the perception of medical schools, such as class size, location, clinical facilities, and other resources. It is extremely difficult to reliably rate medical schools, although the schools listed below are gener- ally considered among the most prestigious. For that reason, admis- sions at these schools are even more competitive than elsewhere. Baylor College of Medicine Columbia University College of Physicians and Surgeons Cornell University Weill Medical College Education and Preparation 15 Duke University School of Medicine Emory University School of Medicine Harvard Medical School Johns Hopkins University School of Medicine Northwestern University Feinberg School of Medicine Stanford University School of Medicine University of California, Los Angeles Geffen School of Medicine University of California, San Diego School of Medicine University of California, San Francisco School of Medicine University of Michigan Medical School University of Pennsylvania School of Medicine University of Pittsburgh School of Medicine University of Texas Southwestern Medical School University of Washington School of Medicine Vanderbilt University School of Medicine Washington University School of Medicine Yale University School of Medicine A list of all 125 U. You will have a better chance of being accepted if you carefully research schools before you choose the ones to which you apply. Most state university medical schools give preference to state residents; some do not accept any out-of-state students. If your state does not have a state-supported medical school (Alaska, Delaware, Idaho, Maine, Montana, New Hamp- shire, Rhode Island, Wyoming), inquire if the state has an agree- ment with a medical school in a neighboring state that would give 16 Opportunities in Physician Careers you preference. The more you know about the process of applying to medical school, the better your chances of admission. During High School Some people know from a very young age that medicine will be their future path. It makes sense to find out early if you like and can handle the rigorous premedical courses necessary to get into medical school. You should take difficult science courses, such as advanced place- ment courses, while still in high school. Good grades and good study habits are important elements for preparing for a future in medicine. Medical school is a long and arduous process that takes more hard work than perhaps any other professional training.
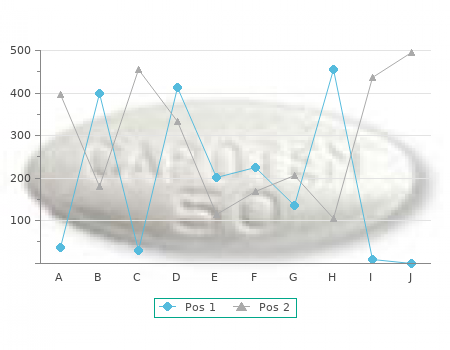
Oral intolerance and severe discomfort requiring hospitalization may accompany large first-degree burns purchase 100 mg furosemide free shipping. These burns have a red cheap furosemide 100mg fast delivery, hyperemic appearance of the surface buy cheap furosemide 100mg online, which discount furosemide 40mg, along with the hypersensibility and discomfort, is typical of these injuries (see Fig. Second-degree burns, also called partial-thickness burns, involve variable amounts of dermis (see Fig. Second-degree burns are subdivided into superfi- cial and deep second-degree wounds. In superficial second-degree burns, the epidermis and the superficial (papillary) dermis have been damaged. A moist, pink appearance that blanches with pressure, along with extreme pain and hyperesthesia, is common in these injuries. Regeneration occurs by proliferation of epithelial cells from hair follicles and sweat gland ducts. Heal- ing is almost complete within 3 weeks, leaving no scarring if no complications occur. In deep second-degree burns, however, the epidermis, papillary dermis, and various depths of the reticular (deep) dermis have been damaged. Complete healing take more than 3 weeks and scarring and infection are common. These injuries are best treated surgically, since excision of the dead tissue and skin grafting shorten hospital stay and improve outcomes. Deep second-degree burns tend to be hypoes- thetic, presenting with less pain than superficial burns. They have a white–pink appearance and blistering does not normally occur, or is present many hours after the injury. A B FIGURE6 The laser Doppler scanner (A) is helpful for the diagnosis of burn wound depth. Its sensitivity and specificity are best between 48 and 72 h after the injury. It is placed over the area to be scanned (B), and in few seconds it produces a digitized image of the burn wound. Typical ap- pearance is that of a hyperemic area with severe discomfort and hyperestesia. Such burns do not blister, and they generally desquamate between 4 and 7 days after injury. Initial Management and Resuscitation 19 A B FIGURE 8 Second-degree burn injuries (or partial-thickness burns) present with different degrees of damage to the dermis. They usually blach with pressure and do not usually leave any permanent scarring. Deep portions of the dermis have been damaged and they tend to leave permanent changes on the skin (C, D). Initial Management and Resuscitation 21 In contrast to the former injuries, third degree burns or full-thickness burns never heal spontaneously, and treatment involves excision of all injured tissue (Fig. In these injuries, epidermis, dermis, and different depths of subcutaneous and deep tissues have been damaged. Pain involved is very low (usually with marginal partial-thickness burns) or absent. In infants and patients with immersion scalds, the burns may appear cherry red, and they may be misleading in nonexperienced hands. Burns that affect deep structures, such as bones and internal organs, are categorized as fourth-degree burns. These injuries are typical of high-voltage electrical injuries and flammable agents, and have a high mortality rate.
Toward an empirically-derived taxonomy of chronic pain pa- tients: Integration of psychological assessment data furosemide 40mg fast delivery. Dysfunctional TMD pa- tients: Evaluating the efficacy of a tailored treatment protocol purchase furosemide 40 mg with visa. Adaptation to metastatic cancer pain buy furosemide 40 mg otc, regional/local cancer pain and non-cancer pain: Role of psychological and behavioral factors order furosemide 40 mg amex. CHAPTER 9 Psychological Interventions for Acute Pain Stephen Bruehl Ok Yung Chung Department of Anesthesiology, Vanderbilt University School of Medicine The importance of optimizing the clinical management of acute pain has been increasingly recognized (Carr & Goudas, 1999). For example, in the context of surgery, providing adequate acute pain control minimizes length of stay and improves outcomes (Kiecolt-Glaser, Page, Marucha, MacCallum, & Glaser, 1998; Ballantyne et al. Postsurgical pain and associated psychological stress can have negative effects on the immune system and endocrine func- tion that impact on recovery (Kiecolt-Glaser et al. Moreover, uncon- trolled nociceptive input may over time result in pathological changes in the central nervous system that could contribute to pain chronicity (e. This central sensitization phenomenon may help explain findings that greater acute pain severity predicts transi- tion to chronic pain (Murphy & Cornish, 1984), and that earlier aggressive management of acute pain may reduce the incidence of postsurgical chronic pain (Senturk et al. Overall, the results just described underscore the fact that effective management of acute postsurgical pain can have a significant impact on outcomes. Adequacy of pain control may also be an important issue to consider with regard to less invasive painful medical procedures. Optimal acute pain control in this latter context may increase tolerability of necessary procedures and impact on willingness to engage in similar procedures in the future (e. Although some clinical acute pain stimuli clearly call for pharmacologi- cal intervention due to their severity (surgery), for other clinical sources of 245 246 BRUEHL AND CHUNG acute pain, such as injections and painful diagnostic procedures, exclusive reliance on pharmacological interventions may not be considered neces- sary or desirable given the brief duration of the pain, risk of side effects, or need for patients’ conscious awareness (e. Vari- ous psychologically based pain management interventions have been de- scribed for use in common clinical situations that result in acute pain (e. Although not intended to be an exhaus- tive review of the literature, this chapter describes a number of the tech- niques available and will overview evidence for their efficacy based on con- trolled clinical trials. Studies examining use of these interventions in comparison to or in conjunction with pharmacological analgesia will be summarized. Finally, issues involved in the practical use of such interven- tions in the clinical setting will be addressed. TYPES OF INTERVENTIONS Substantial research following the gate control theory of pain described by Melzack and Wall (1965) has confirmed the presence of descending neuro- physiological pathways through which psychological states can either ex- acerbate or inhibit afferent nociceptive input and the experience of pain. Al- though extreme emotional distress may be associated with stress-induced analgesia (Millan, 1986), at less extreme levels, greater emotional distress is generally associated with increased acute pain intensity (Graffenreid, Adler, Abt, Nuesch, & Spiegel, 1978; Litt, 1996; Sternbach, 1974; Zelman, Howland, Nichols, & Cleeland, 1991). Psychological strategies for managing acute pain therefore often intervene at the cognitive and physiological level to reduce distress and arousal that may lead to heightened experience of acute pain (Bruehl, Carlson, & McCubbin, 1993). In addition, the simple fact that a specific pain management technique has been provided is likely to in- crease patients’ perceived sense of control, which also appears to be an im- portant factor in reducing negative responses to painful stimuli (Litt, 1988; Weisenberg, 1987). Available psychological techniques for management of acute pain can be broadly categorized into information provision, relax- ation and related techniques, and cognitive strategies (e. Although some interventions, such as information provision, are primarily preemptive and designed to minimize pain by preparing the patient for what will be experienced, others such as relaxation techniques may be useful both preemptively and for reducing acute pain as the patient is experiencing it. Common psychological pain management techniques are summarized in Table 9. Relaxation related Breathing relaxation Simplest relaxation technique to implement. Progressive muscle relaxation Effective but may require re- peated training/practice ses- sions. Imagery Can use scripted, patient- developed, or memory-based relaxing imagery. Hypnosis Combines elements of relax- ation and imagery + sugges- tions of analgesia or sensory transformation. Distraction Includes visual or auditory stimuli, or mental and behav- ioral tasks that divert atten- tion away from pain.
Dissatisfaction with biomedical approaches is reflected in the ma- jor resurgence of interest in alternative and complementary medicine and the substantial market share of health expenditures this sector has been able to capture in providing services to chronic pain patients who have not benefited from conventional western medical care order furosemide 100mg online. Essentially generic 100 mg furosemide overnight delivery, failures of Western approaches to health care and urgent need for relief from pain have led to free-market competition cheap 100 mg furosemide otc. PSYCHOLOGICAL PERSPECTIVES: CONTROVERSIES 305 vantageous safe 40 mg furosemide, as it encourages exploration of new ideas and diffusion of inno- vation on an essentially global basis. The psychological perspective on pain offers considerable promise, and there have been substantial advances since Sternbach (1968) published the first book representing a synthesis in the area. Most major health problems (cardiovascular disease, musculoskeletal disorders, diabetes, obesity, HIV- AIDS, cancer) are largely due to psychosocial and lifestyle factors. The fo- cus of medicine is on management of disease, with the medical profession not effectively addressing behavioral health issues or pain arising from many conditions. The well-being of patients would seem to dictate stronger alliances between primary care physicians, other health care professionals, and psychologists. Our task in this chapter is to identify contentious issues, both those al- ready recognized and others that became apparent as we surveyed the field. Having noted this, we recognize that this ac- count represents a subjective perspective. Not everyone would recognize the same controversies, and we would encourage those who do not agree with our concerns to describe the issues that are problematic for them. THE NATURE OF PAIN AND CONTROVERSIES ABOUT ITS DEFINITION As amply demonstrated in the earlier chapters of this volume, concepts of pain have evolved dramatically throughout the last century. Sensory-spe- cific models proved unable to explain many of the complexities of pain (see Melzack & Wall, 1996 for an overview) and yielded to multidimensional models that acknowledge pain as a complex synthesis of thoughts, feelings, and sensory input, as described in the chapter by Melzack and Katz in this volume as well as in the work of others. For example, Price (2000) showed that the cortico-limbic pathway in the brain integrates nociceptive input with contextual information and memory to provide cognitive mediation of pain affect. There is no need here to review the history or the basis for the advances in thinking, although the transformations in thinking have not fully pervaded the practice of working with pain patients. While there would be agreement that considerable pain is suffered need- lessly (Melzack, 1988), one might generate the argument that not all pain is undesirable. Advocates of corporal punishment and those who practice vio- lence appear to perceive merit in inflicting pain to punish or modify the be- havior of others. Evidence of its limited effectiveness and the unfortunate consequences of misuse of punishment (Gershoff, 2002) do not seem to in- hibit its use. Others argue that personal experiences of pain have beneficial consequences. Few would disagree that pain serves to warn of injury and 306 CRAIG AND HADJISTAVROPOULOS disease. The consequences of congenital insensitivity to pain are well known (Melzack, 1973): The injuries sustained and diseases not averted have the potential to cause early death. Anthropological literature rein- forces the idea that pain is desirable under certain circumstances. In some religious perspectives, pain can be a source of divine experience and im- portance (Tu, 1980). The current popularity of tattooing, body piercing, and even self-inflicted branding signals a willingness to tolerate pain for per- sonal outcomes. Pain during masochistic sexual rituals illustrates how so- cial contextual factors can transform the pain experience. Religious peni- tents who subject themselves to flagellation, fire-walking, body piercing and mutilation, and even death (Glucklich, 2000) display a dramatic willingness to self-inflict pain. These examples illustrate the human capacity to over- ride biological imperatives to avoid pain in the interests of personal values. These varying social contexts highlight the importance of value judgments in appraisals of the role of pain in human experience. The widely used and accepted definition of pain created by the Interna- tional Association for the Study of Pain (1979), has been a powerful influ- ence in our understanding.
