

V. Gunnar. State University of New York Institute of Technology at Utica/Rome.
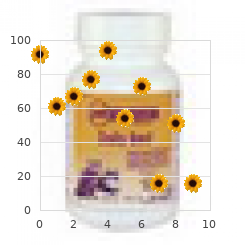
Everman generic 100mcg rhinocort with visa, MD with BD has signs or symptoms of another underlying condition proven rhinocort 100 mcg, certain laboratory tests may be recommended order rhinocort 100 mcg online. These tests may identify other associated medical prob- lems or help to pinpoint a specific diagnosis cheap rhinocort 100mcg line. IBranchiootorenal syndrome Treatment and management Definition Many people who have BD are perfectly healthy and Branchiootorenal (BOR) syndrome is an autosomal do not require any specific treatment for their hands and dominant condition characterized by ear abnormalities, feet. When use of the hands is impaired, physical therapy hearing loss, cysts in the neck, and kidney problems. Evaluation by an orthopedist or physical therapist Description may also be helpful for people who have trouble walking comfortably due to bone changes in the feet. Surgery can The name branciootorenal syndrome describes the be used to lengthen the hand or foot bones in some severe body systems most commonly affected by this genetic forms of BD. The term “branchio” refers to the abnormalities have significant clinodactyly, syndactyly, or sympha- of the neck found in individuals with this syndrome. For example, the Autosomal dominant—A pattern of genetic inher- outer ear can be unusual in appearance. These can be very mild or very severe, as can any of body or both of a pair of organs. Melnick first described branchiootorenal Cleft palate—A congenital malformation in which (BOR) syndrome in 1975. Another name for BOR syn- there is an abnormal opening in the roof of the drome is Melnick-Fraser syndrome. Individuals with mouth that allows the nasal passages and the BOR syndrome typically have physical differences that mouth to be improperly connected. These birth defects are Congenital—Refers to a disorder which is present caused by a change (mutation) in a gene. Cyst—An abnormal sac or closed cavity filled with Genetic profile liquid or semisolid matter. Scientists recently discovered that mutations in the Deoxyribonucleic acid (DNA)—The genetic EYA1 gene cause BOR syndrome. The EYA1 gene is material in cells that holds the inherited instruc- located on chromosome 8. The exact function of the tions for growth, development, and cellular func- EYA1 gene is unknown, but mutations in this gene dis- tioning. The branchial arches are Fistula—An abnormal passage or communication tissues that develop very early in pregnancy and are between two different organs or surfaces. Gene—A building block of inheritance, which BOR syndrome is inherited in a dominant manner. Each gene is son has a mutation in one of their EYA1 genes, the dis- found on a precise location on a chromosome. The characteristics of the Gustatory lacrimation—Abnormal development syndrome can be extremely variable in severity. A mutation can also occur by chance, in an individual without a family history of Microtia—Small or underdeveloped ears. If a child inherits an abnormal gene Mutation—A permanent change in the genetic from a parent, the signs of the disorder can be very dif- material that may alter a trait or characteristic of ferent between the parent and the child. This is called an individual, or manifest as disease, and can be variable expressivity. Once an individual has a mutation in the EYA1 gene, there is a 50/50 chance with each pregnancy that the gene Renal agenesis—Absence or failure of one or both will be passed on. It does not matter if the gene Unilateral—Refers to one side of the body or only is inherited from the mother or the father. Variable expressivity—Differences in the symp- Demographics toms of a disorder between family members with BOR syndrome occurs in one of every 40,000 live the same genetic disease. BOR syndrome is seen in all ethnic groups and GALE ENCYCLOPEDIA OF GENETIC DISORDERS 171 Branchiootorenal Syndrome Hearing loss Cleft palate Bifid uvula Hearing loss Hearing loss Polycystic kidneys Hearing loss Hearing loss Hearing loss Branchial cleft cyst Cleft palate Kidney problem One kidney missing (Gale Group) cultures. One abnormally shaped, malfunctioning, or totally absent study suggested that 2% of individuals with severe hear- (renal agenesis). Other less common characteristics associated with BOR syndrome include cleft palate, facial nerve paraly- sis, and abnormalities of the tear ducts. Some The characteristics associated with BOR syndrome patients with BOR syndrome uncontrollably develop are highly variable.

Although these formulas have been shown to normalize the amino acid 12 profile and in some cases improve nitrogen balance generic rhinocort 100mcg with visa, no studies have demonstrated an im- proved patient outcome buy discount rhinocort 100 mcg. The additional cost of these formulas is a deterrent to their routine use in these populations until further data are available order 100 mcg rhinocort visa. Studies have shown losses to be increased in stress; therefore order 100mcg rhinocort overnight delivery, daily supplementation of up to 15 mg of zinc may be appropriate. COMMON TPN COMPLICATIONS Hyperosmolar Nonketotic Coma: Usually found in improperly monitored patients with impaired insulin responses. Caused by excessive glucose levels, usually corrected by administration of insulin and rehydration. Sustained hyperglycemia (>220 mg/dL) depresses monocyte activity and could compromise the immune defenses. If the patient becomes septic, the deep line should be considered a possible source. If no other source of infection can be identified, the deep line must be removed or changed and the tip sent for routine cul- ture and sensitivity. Candida albicans is the most frequently encountered pathogen on the catheter, followed by Staphylococcus aureus, Staphylococcus epidermidis and gram- negative rods. Hypophosphatemia: Severe hypophosphatemia can occur in patients started on TPN after severe weight loss and those with conditions such as anorexia nervosa (refeeding syn- drome). This may also result from increased metabolic processes requiring phosphate and can significantly hamper weaning from the ventilator. When the primary metabolic pathway for glucose becomes saturated, excess glucose is converted to intracellular triglycerides in the liver. Cholestasis: This often occurs secondary to overfeeding of fat calories (>3 g/kg/d or >60% of total nonprotein calories). Most TPN formulations contain potassium 40–50 mEq/L and are intended for patients with nor- mal renal function. Excess potassium over and above that required for maintenance and urine losses (usually 3–5 mEq/g nitrogen) is included. Potassium must be closely followed in the elderly and those with impaired renal function. These include some antibiotics that are potassium salts (eg, penicillins); oral phosphate supplements (Neutra-Phos); ACE inhibitors, which reduce potassium excretion (Captopril, Enalapril); and potassium-sparing diuretics (triamterene, spironolactone). Metabolic Alkalosis: Modern SAAs are present as the acetate salt (80–100 mEq/L), which is converted to bicarbonate in vivo. In postoperative patients with nasogastric tubes, the loss of chloride, together with the high infusion of the acetate, can lead to a metabolic al- kalosis. The increased use of histamine blockers and antacids in intensive care patients has also contributed to a higher incidence of this problem. Treating this condition requires in- creasing the chloride level in the solution and reducing the acetate. Hyponatremia: Serum sodium levels of 127–135 mEq/L are commonly seen in patients on TPN. The cause is controversial but is probably due to mild SIADH; therefore the prob- 12 lem is probably an excess of water and not deficiency of sodium. It is usually asymptomatic and does not require a change in formula unless the sodium drops below 125 mEq/L. Not all patients infected with transmissible pathogens can be identified at the time of hospital admission or even later in their course. Because pathogens transmitted by bloody and body fluids pose a hazard to personnel caring for such patients, particularly during invasive procedures, certain precautions are now required for routine care of all patients whether or not they have been placed on isolation precautions of any type. For ex- ample, wear gloves for all venipunctures, for all IV starts, for IV manipulation, and for wound care. Do not wear the same pair to perform tasks on two dif- ferent patients or two different tasks at different sites on the same patient. Wear gloves in every instance in which contact with any body fluid is likely, including urine, feces, wound secretions, respiratory tract care, thoracentesis, paracentesis, etc. Additional barrier precautions may be necessary for certain invasive procedures when significant splatter or aerosol generation seems likely. It may occur in certain instances in the operating room, emergency room, the ICUs, during invasive procedures, and during cardiopulmonary resuscitation.

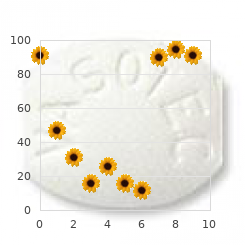
If absorbable (5-0 or 6-0 Dexon or Vicryl) is used order 100mcg rhinocort fast delivery, the knot is usually buried as shown discount 100 mcg rhinocort amex. Hands must be crossed at the end of the first loop tie (step F) to give a flat knot; hands are not crossed at the end of the second loop tie (step J) order rhinocort 100 mcg fast delivery. Begin with either a single or double (illustrated) looping of the lower end of the suture around the needle holder buy generic rhinocort 100 mcg on-line. Hands must be crossed after the second loop tie (step G) to produce a flat square knot. Be sure that the staple is completely “re- formed” before removal to decrease patient discomfort. It is useful in wounds that are clean and easily op- posed and for young children, for whom suture removal may be a problem. It is also useful for stabilizing wounds if the sutures were removed very early in order to minimize suture marks. It should not be used for puncture wounds, bites or wounds that need debridement, or in regions subjected to frequent movement (ie, hand or finger). After 2–3 min (after the glue has dried), an additional one or two coats may be applied. Once the glue is in place and stable, it is not necessary to use any topical medication or oint- ment. The objective is the treatment and care of all types of patients with cardiopulmonary diseases. Functions of the respiratory therapist include emergency care, ventilatory support, airway management, oxygen therapy, humidity and aerosol therapies, chest physiotherapy, physiologic monitoring, and pul- monary diagnostics. PULMONARY FUNCTION TESTS PFTs are useful in diagnosing a variety of pulmonary disorders. Common PFTs include spirometry, lung volume determinations, and diffusing capacity. Spirometry may identify obstructive airway diseases such as asthma or emphysema when the ratio of FEV1/FVC is less than 70%, or restrictive lung diseases such as sarcoidosis or ankylosing spondylitis when both the FVC and FEV1 are reduced. Spirograms can be obtained before and after the administration of bronchodilators if they are not contraindi- cated (ie, history of intolerance). Bronchodilator responsiveness will help in predicting the response to treatment and in identifying asthma. Lung volumes commonly determined by helium dilution must be ordered to definitively diagnose restrictive lung disease. Diffusion capacity is important in the diagnosis of interstitial lung disease or pulmonary vascular disease, where it is reduced. It is also frequently followed to determine the response to therapy in interstitial diseases. Obstructive pulmonary diseases include asthma, chronic bronchitis, emphysema, 18 bronchiectasis, and lower airway obstruction. Restrictive pulmonary disease includes inter- stitial pulmonary diseases, diseases of the chest wall, and neuromuscular disorders. Intersti- tial disease may be due to inflammatory conditions [usual interstitial pneumonitis (UIP)], inhalation of organic dusts (hypersensitivity pneumonitis), inhalation of inorganic dusts (as- bestosis), or systemic disorders with lung involvement (sarcoidosis). Normal values for a given patient are established from studies of normal populations and are provided along with the results. Tidal Volume (TV): Volume of air moved during a normal breath on quiet respiration 18 Forced Vital Capacity (FVC): Maximum volume of air that can be forcibly expired after full inspiration Functional Residual Capacity (FRC): Volume of air in the lungs after a normal tidal expiration (FRC = reserve volume + expiratory reserve volume) Total Lung Capacity (TLC): Volume of air in the lungs after maximal inspiration Forced Expired Volume in 1 Second (FEV1): Measured after maximum inspira- tion, the volume of air that can be expelled in 1 s 18 Respiratory Care 361 Vital Capacity (VC): Maximum volume of air that can be exhaled from the lungs after a maximal inspiration Residual Volume (RV): The volume of air remaining in the lungs at the end of a maxi- mal exhalation DIFFERENTIAL DIAGNOSIS OF PFTS Table 18–1 shows the differential diagnosis of various PFT patterns. When interpreting PFTs, remember that some patients may have combined restrictive and obstructive diseases such as emphysema and asbestosis. OXYGEN AND HUMIDITY SUPPLEMENTS Table 18–2 describes various methods of oxygen and humidity supplementation. TABLE 18–1 Differential Diagnosis of Pulmonary Function Tests Restrictive Obstructive Test Disease Disease FVC ↓ N or ↓ TLC FEV1/FVC N or FEV1 OBSTRUCTIVE AIRWAYS DISEASE (COPD) Test Normal Mild Moderate Severe FEV1 (% of VC) >75 60–75 40–60 <40 RV (% of predicted) 80–120 120–150 150–175 >200 RESTRICTIVE LUNG DISEASE Test Normal Mild–Moderate Severe 18 FVC (% of predicted) >80 60–80 50–60 <50 FEV1 (% of VC) >75 >75 >75 >75 RV (% of predicted) 80–120 80–120 70–80 70 Abbreviations: N = normal; ↑ = increased, ↓ = decreased; FVC = forced vital capacity; TLC = total lung capacity; RV/FRC = residual volume/functional residual capacity; FEV1 = forced expiratory volume in 1s; VC = vital capacity.
Your doctor will do a physical examination including the fol- lowing: blood pressure generic rhinocort 100mcg with amex, pulse 100 mcg rhinocort visa, pushing on the abdomen order rhinocort 100mcg without a prescription, checking for stability in the bones of the pelvis trusted 100 mcg rhinocort, digital rectal exam, checking stool for the presence of blood. FACTOR WHAT IS IT YPICAL SYMPTOMS Internal Damage to internal Abdominal pain, tender- damage or organs as a result of ness, bruising, blood in bleeding injury urine, more common after a penetrating wound Pelvic Pain or Injury What your doctor will ask you about: blood in urine, inability to urinate, numbness or decreased strength in legs and feet. FACTOR WHAT IS IT YPICAL SYMPTOMS Pelvic fracture A break in one of the Pain on weight bearing or bones of the pelvis direct pressure to pelvis, change in strength and sensation in legs, blood in urine Urethral tear A tear in the tissues of Blood in urine, inability to the urethra, which drains urinate urine from the bladder Injury to Arms or Legs Your doctor may ask you to remove any jewelry or clothing that could become constrictive if your injured limb begins to swell. Your doctor will do a physical examination including the follow- ing: pulse, temperature, sensation and movement in the injured limb, testing joints for mobility and stability, checking joints for swelling, testing for broken bones. FACTOR WHAT IS IT YPICAL SYMPTOMS Nerve or vessel Damage to nerves or Loss of sensation or move- injury blood vessels in the ment in the injured limb, injured limb pallor, coldness Fracture or A break in one of the Loss of function in the dislocation bones of the injured limb injured limb, tenderness, swelling Open fracture Bone protrudes through Bone protrudes through the the skin skin INJURY 129 Neck or Back Injury and Back Pain What your doctor will ask you about: weakness, loss of sensation in arms or legs, pain in the neck or back, trouble moving the back or spine, blood in urine, inability to urinate. Your doctor will do a physical examination before you are moved after your injury. The exam will include the following: checking neck and back for tenderness and alignment, looking for tenderness in the spine and along the sides of the body, pushing on the abdomen, testing reflexes and sensation. CAUSE WHAT IS IT YPICAL SYMPTOMS Muscle strain Reversible injury to the Sudden onset after muscles that can occur strenuous activity, after lifting heavy objects; pain does not move to legs this is the cause of about 70% of back pain Arthritis Inflammation of the joints Pain is usually present in extremities as well as back Herniated disk Abnormal bulging of the Difficulty moving legs, spongy disks that keep worsened by coughing the spinal bones properly or sneezing, may involve spaced difficulty urinating, some- times follows spine fracture (see below) Spine fracture A break in one of the Neck or back pain vertebrae, often due to osteoporosis, which primarily affects women after menopause Spinal stenosis Narrowing of the space in Low back pain moving to the bones in which the the thighs (pain may be spinal cord sits relieved by bending for- ward), thigh weakness, unsteady gait Major Injury to one of the nerves Loss of sensation in the neurological that comes out of the extremities, difficulty deficit spine and travels to the urinating extremities 130 INJURY WHAT ARE SOME CAUSES OF NECK OR BACK INJURY OR BACK PAIN? Childhood irritability can occur when a child feels badly because of disease or experiences problems coping with life changes or other aspects of his environment. Your Doctor Visit What your doctor will ask you about: headache, stiff neck, fever, ear pulling, salivation, nausea, vomiting, changes in appetite, diar- rhea, crying when urinating, coughing, wheezing, difficulty breath- ing, skin rash, changes in weight, excessive crying, difficulty reading, attitudes toward school, hyperactivity. Your doctor will want to know if the child has had any condi- tions or diseases, including: birth trauma, retardation, seizures (convulsions). Your doctor will want to know what the child refuses to do, the nature of his irritable behavior, his medications, and how he acts differently from other siblings when they were his age. Your doctor will do a physical examination including the fol- lowing: temperature, height, weight, feeling the skull, hearing, eye- sight, looking inside the mouth and throat, listening to the chest and heart with a stethoscope, pushing on the abdomen, testing reflexes and movement, testing developmental skills. CAUSE ASSOCIATED SYMPTOMS Attention deficit/ Difficulty sitting still or paying attention, hyperactivity disorder poor school performance Autism Bizarre or unpredictable behavior, failure to communicate Obsessive-compulsive Frequent checking or repetitive behaviors disorder Meningitis Fever, headache, stiff neck, squinting Ear infection Fever, ear pain Teething Tooth pain, crying spells Seizures Convulsions, uncontrolled shaking, loss of consciousness Dyslexia and learning Difficulty reading and comprehending disorders Deafness Difficulty hearing, or complete deafness Skin conditions Deforming skin conditions, shyness Mental retardation Extreme difficulty comprehending, low IQ Joint Pain What it feels like: pain involving one or more joints, which may extend to muscles. For more information about pain in the hand, wrist, or arms, see the chapter on Hand, Wrist, or Arm Problems. If your pain is only in your foot or ankle, see the chapter on Foot or Ankle Pain. Your Doctor Visit (shoulder or left arm pain) What your doctor will ask you about: chest pain, muscle pain, pain in other joints, pain spreading to other joints. Your doctor will want to know if you or anyone in your family has had any of these conditions: diabetes, high blood pressure, heart disease, past shoulder dislocations, or episodes of bursitis. Your Doctor Visit (hip pain) What your doctor will ask you about: ability to walk, low back pain, muscle pain, pain in other joints, pain spreading to other joints. Your doctor will want to know if you or anyone in your family has had any of these conditions: sickle-cell disease, past surgery on or near hip. Your doctor will want to know if you or anyone in your family has had any of these conditions: hemophilia, past knee injury or surgery. Your Doctor Visit (calf or leg pain) What your doctor will ask you about: muscle pain, pain in other joints, pain spreading to other joints, calf swelling or tenderness, low back pain, pain worsened by coughing. Your doctor will want to know if you or anyone in your family has had any of these conditions: heart disease, chronic lung dis- ease, recent surgery or prolonged immobilization, thrombophlebitis. Your Doctor Visit (general joint pain) What your doctor will ask you about: muscle pain, pain in other joints, pain spreading to other joints, fever, stiffness of joints in the morning, skin lesions, back pain, cough, runny nose, diarrhea, headache, finger pain, discoloration in the cold. Your doctor will want to know if you or anyone in your family has had any of these conditions: rheumatoid arthritis, gout, gon- orrhea, past trauma or surgery to painful area, rheumatic fever, gen- ital discharge. Your doctor will want to know if your pain gets worse at the end of the day or if you feel especially stiff in the morning and, if so, for how long. Your doctor will want to know how long your pain has occurred, and if you were recently exposed to deer ticks or strep throat. JOINT PAIN 135 Your doctor will do a physical examination including the following: • Pain in arms or legs: checking for swelling, tenderness, defor- mity, discoloration or warmth, range of motion.