

By X. Eusebio. Rocky Mountain College.
Antibodies against signal recognition particle (SRP) D order 0.1mg florinef visa. Antibodies against Mi-2 Key Concept/Objective: To know the antibodies that correlate with different clinical pictures in idiopathic inflammatory myopathies Autoantibodies to nuclear and cytoplasmic antigens are found in as many as 90% of patients with an inflammatory myopathy purchase 0.1 mg florinef. These antibodies are often useful in differenti- ating inflammatory myopathies from diseases that are not autoimmune disorders buy discount florinef 0.1mg. Some of these antibodies are nonspecific and can be seen in several autoimmune disorders florinef 0.1mg fast delivery. About 25% of patients with inflammatory myositis test positive for antinuclear antibod- ies. Autoantibodies that are in large part directed against cytoplasmic ribonucleoproteins have been designated as myositis-specific autoantibodies (MSA) and are present in 30% of the patients. These antibodies tend to correlate with some specific clinical presentations, responses to therapy, and prognoses. Three groups of patients can be defined by the MSA specificities. The first group is defined by the presence of antibodies directed against aminoacyl-tRNA synthetases. These patients are generally characterized by an acute onset of muscle disease, with a high incidence of associated interstitial lung disease. They may also have arthritis and a hyperkeratotic rash on the hands, known as mechanic’s hands. This description fits the patient presented in this case. The second group includes patients with anti-SRP antibodies; these patients tend to have an abrupt onset of weakness, and they may have cardiac disease. The third group is identified by the presence of antibodies against Mi-2; these patients have a dermatomyositis with the so-called shawl sign. A 58-year-old man is seen in your clinic for the first time. He says he has decided to see a doctor because over the past 2 years he has noticed some weakness of his arms and legs. He says these symptoms were not bothering him ini- tially but that, over the past few months, he has noticed more weakness in his left arm. On physical examination, there is no rash; his strength is 5/5 on the right side of his body, 5/5 in his left leg, and 3/5 in his left arm. His distal strength and proximal strength are quite sim- ilar. Neurologic examination results are otherwise normal. His creatine kinase (CK) level is moderately elevated. Which of the following is the most likely diagnosis for this patient? Inclusion body myositis (IBM) Key Concept/Objective: To understand the presentation of inclusion body myositis This patient is a middle-aged man with slow-onset muscle weakness. Dermatomyositis is defined by the presence of an inflammatory myopathy and a characteristic rash. Polymyositis is characterized by weakness that is symmetrical and predominantly proxi- mal, and the clinical course is more aggressive than the one described here. Sarcoidosis can cause a myopathy but usually is accompanied by other manifestations that are absent here. This patient’s symptoms are more consistent with IBM. The pattern of severity of muscle weakness in IBM differs from that seen in other idiopathic inflammatory myopathies. In addition to the presence of proximal weakness, distal muscles may be involved, and in some cases, muscle abnormalities are asymmetrical. Unlike most of the other inflammatory muscle disorders, IBM affects more men than women. Electron microscopy may be required to demonstrate the inclusion bodies that define IBM.
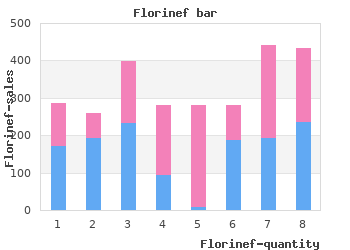
During an attack there is an increase in insertional activity discount florinef 0.1mg on line, and an increase in short duration discount 0.1mg florinef overnight delivery, polyphasic motor unit potentials that disappear as the muscle be- comes paralyzed cheap 0.1 mg florinef amex. In most subjects the needle EMG is normal between attacks florinef 0.1 mg free shipping. Muscle biopsy: Clear central vacuoles are observed, along with tubular aggregates. In addition, there may be myopathic changes including variation in muscle size, split fibers, and internalized nuclei. There is vacuolar dilation of the sarcoplasmic reticu- lum during attacks. Acetazolamide sustained release tablets (500–2000 mg/d) or dichlorphenamide (50–150 mg/d) may reduce the frequen- cy of the attacks. Use of potassium sparing diuretics (triamterene or spironolac- tone) in combination with acetazolamide or dichlorphenamide may also re- duce the frequency of periodic paralysis. With appropriate treatment the prognosis is usually good. Prognosis Cannon SC (2002) An expanding view for the molecular basis of familial periodic paralysis. References Neuromuscul Disord 12: 533–543 Davies NP, Eunson LH, Samuel M, et al (2001) Sodium channel gene mutations in hypokalemic periodic paralysis: an uncommon cause in the UK. Neurology 57: 1323– 1325 Dias da Silva MR, Cerutti JM, Tengan CH, et al (2002) Mutations linked to familial hypokalaemic periodic paralysis in the calcium channel alpha1 subunit gene (Cav1. Clin Endocrinol (Oxf) 56: 367–375 Lehmann-Horn F, Jurkat-Rott K, Rudel R (2002) Periodic paralysis: understanding channel- opathies. Curr Neurol Neurosci Rep 2: 61–69 Moxley III RT (2000) Channelopathies. Curr Treat Options Neurol 2: 31–47 439 Motor neuron disease 441 Amyotrophic lateral sclerosis Genetic testing NCV/EMG Laboratory Imaging Biopsy + Fig. Progression of ALS may impose severe communication- al problems. Dysarthria and in- ability to speak can be com- pensated in some patients with computer devices, such as spe- cial keyboards and a mouse Amyotrophic lateral sclerosis (ALS) causes the loss of both upper and lower Anatomy motor neurons. On autopsy, there is loss of the pyramidal cells of the motor cortex, with atrophy of the brainstem and spinal cord. The corticospinal tracts are degenerated and gliotic. The ventral nerve roots are atrophied, and there is microscopic evidence of muscle denervation and reinnervation. ALS usually presents with painless and progressive weakness of a focal distribu- Symptoms tion that over time spreads to contiguous muscle groups. As the disease progresses, fasciculations cause muscle cramps and the patient becomes spas- tic. Weakness can lead to head drop, and contractures can lead to hand and foot deformaties. Bulbar symptoms may be the presenting feature of ALS, but more commonly patients present with trunk and extremity weakness. Dysarthria is common and may be spastic or flaccid, or a combination of both. Dysphagia puts patients at a high risk for choking and aspiration. Spontaneous swallowing is absent, leading to drooling (sialorrhea). Respiratory weakness is rarely the presenting feature of ALS, but becomes common with disease progression. Patients initially experience exertional dys- pnea and sigh frequently when at rest. This continues on to dyspnea at rest, sleep apnea, morning headaches, and the inability to sleep supine. Nearly one third of ALS patients report urgent and obstructive micturition. Over time, muscles become atrophied and patients complain of fatigue.
On this medial view generic florinef 0.1 mg with mastercard, the thalamic portion of the diencephalon is separated from the hypothalamic part by CEREBRAL HEMISPHERES 7 a groove florinef 0.1mg generic, the hypothalamic sulcus buy 0.1 mg florinef with mastercard. This sulcus starts at the foramen of Monro (the interventricular foramen 0.1mg florinef otc, dis- cussed with the ventricles, see Figure 20A and Figure CEREBRAL HEMISPHERES: MEDIAL 20B) and ends at the aqueduct of the midbrain. The optic (PHOTOGRAPHIC) VIEW chiasm is found at the anterior aspect of the hypothalamus, and behind it is the mammillary body (see Figure 15B). This view of the brain sectioned in the midline (mid- The three parts of the brainstem can be distinguished sagittal plane) is probably the most important view for on this view — the midbrain, the pons with its bulge understanding the gross anatomy of the hemispheres, the anteriorly, and the medulla (refer to the ventral views diencephalon, the brainstem, and the ventricles. Through the midbrain tion has divided the corpus callosum, gone in between the is a narrow channel for CSF, the aqueduct of the midbrain thalamus of each hemisphere (through the third ventricle), (see Figure 20A and Figure 20B). The midbrain (behind and passed through all parts of the brainstem. The central fissure does extend onto this part of Figure 18). The medial surface of the frontal lobe is situated fourth ventricle, a space with CSF that separates the pons anterior to the fissure; the inferior gyri of the frontal lobe and medulla from the cerebellum (see Figure 20A and sit on the bone that separates the anterior cranial fossa Figure 20B). CSF escapes from the ventricular system at from the orbits (see Figure 15A and Figure 15B). The the bottom of the fourth ventricle through the foramen of parietal lobe lies between the central fissure and the deep Magendie (see Figure 21), and the ventricular system con- parieto-occipital fissure. The occipital lobe is now vis- tinues as the narrow central canal of the spinal cord (see ible, posterior to this fissure. It has been sectioned through its midline portion, along its banks (see Figure 41A and Figure 41B). Although it is not necessary The corpus callosum in this specimen has the expected to name all of its various parts, it is useful to know two “white matter” appearance. Inside each cerebral hemi- of them — the lingula and the nodulus. The tonsil of the cerebellum can also be membranous septum that divides the anterior portions of seen in this view (not labeled, see Figure 9B and Figure the lateral ventricles of one hemisphere from that of the 56). The fornix, a fiber tract of the limbic the occipital lobe. One of the dural venous sinuses, the system, is located in the free lower edge of the septum. This view clarifies the separation of the important gyrus of the limbic system (see Figure 70A). Figure 20B), thereby revealing the diencephalic region. The pituitary gland is situated within the pituitary bony fossa, the sella turcica (see Figure 21). MRI: T1 SAGITTAL VIEW (RADIOGRAPH) Below the thalamus is the brainstem — its three parts, midbrain, pons, and medulla, can be identified. The tectum This radiological image, obtained by magnetic resonance imaging (MRI), shows the brain as clearly as the actual (with its four colliculi) is seen behind the aqueduct of the brain itself (review the NOTE on radiologic imaging with midbrain (see Figure 21). Posterior to the tectum is a CSF cistern (see Figure 28A, the guadrigeminal cistern). This is the way the brain will be seen in the fourth ventricle separates the cerebellum from the pons clinical setting. Note that the CSF is dark in this image, and medulla. The medulla ends at the foramen magnum and becomes the spinal cord. The bones (tables) of the skull are The cerebellar folia are quite distinct on this image. The location of the cerebellar tonsil(s) should be noted, visible as a dark space, while the bone marrow, including adjacent to the medulla and immediately above the fora- its replacement by fatty tissue, and layers of soft tissue (and fatty tissue) of the scalp are well demarcated (white).

A two-point contact condition was maintained until about 66° of knee flexion order florinef 0.1mg fast delivery. From there on cheap florinef 0.1 mg, and until 90° of flexion order 0.1 mg florinef mastercard, a one-point contact was predicted on the medial side florinef 0.1mg fast delivery. This motion is expected and can be thought of as a result of the femur rotating externally over fixed plateaus which causes the medial tibial contact point to move anteriorly and the lateral tibial contact point to move posteriorly. The analysis show that the position of separation in the lateral compartment was slightly affected by the amplitude and/or duration of the forcing pulses. However, the motion pattern of the medial and lateral femoral and tibial contact points was independent of both pulse amplitude and pulse duration. Henceforth, the medial shift velocity increased, reaching a maximum at 90° of knee flexion. Then, the varus velocity increased, reaching a maximum between 40 and 50° of knee flexion; henceforth, the velocity decreased reaching zero between 60 and 65° of knee flexion. The valgus velocity increased again achieving a maximum around 80° of knee flexion. Then, the external rotation velocity began to increase reaching a maximum at around 8° of knee flexion and decreased, reaching zero around 20° of knee flexion. From this point, the internal rotation velocity increased to a maximum between 45 and 60° of knee flexion then decreased as the knee flexion increased. The remaining results related to contact and ligamentous forces are shown for pulses of different amplitudes and a constant duration of 0. These two figures show that increasing the pulse amplitude caused a decrease in the magnitude of the medial and lateral contact forces; similar results were obtained when the pulse duration was increased while the pulse amplitude was kept unchanged. As the flexion angle increased, this tension decreased while tension in the anterior fibers increased and became dominant. The maximum forces in the anterior and deep fibers occurred between 40 and 50° of knee flexion, while the maximum force in the oblique fibers occurred at approximately 5° of knee flexion. The results show that the patterns of change in the ligamentous forces were not generally affected by changing the characteristics of the applied pulsing loads. However, increasing pulse amplitude (and/or duration) slightly affected the magnitude of the forces in the different ligamentous fibers. The procedure is then repeated at different positions to cover a range of knee motions. However, these quasi-static models cannot predict the velocity or acceleration of the different segments forming the joint. Also, these models are further limited in that they cannot determine the effects of the dynamic inertial loads (which occur in many daily living activities) on joint kinematics and joint loads. In this chapter, a © 2001 by CRC Press LLC FIGURE 1. The system of equations forming an anatomical quasi-static knee model is a system of nonlinear algebraic equations. These equations are solved iteratively using a Newton-Raphson iteration tech- nique,20-23,129,130 discretized and solved using the finite element method9 or rewritten as a potential energy function that can be minimized using an optimization method such as the steepest descent optimization technique. Solving a DAE system is more difficult than solving an algebraic system. Several techniques have been proposed to solve the DAE system that describes the two-dimensional dynamic response of the knee joint. Using the Differential/Algebraic System Solver software (DASSL) developed at the Lawrence Livermore National Laboratory, the latter and more complex DAE system was solved, thus describing the three-dimensional dynamic response of the knee joint. The integration scheme implemented in DASSL employs variable order and variable size multistep backward differentiation formulas (BDFs). It is hard to validate the present model predictions because of the limited experimental data available in the literature that describe the dynamic behavior of the human knee joint. The dynamic response of the joint must be described in terms of the loads exerted on the joint; the six components of the three- dimensional motion of the tibia with respect to the femur; the deformations of the different components forming the joint, including the ligaments, menisci and cartilage. Varus-Valgus Rotation Model predictions show that varus rotation occurred in association with internal tibial rotation while the knee was flexed.
It is estimated that worldwide over two million bone grafting procedures are performed annually discount florinef 0.1mg online. As the demand for these procedures continues to increase cheap florinef 0.1mg without prescription, it will place a strain on the limited supply of graft material 0.1 mg florinef otc. Successful bone regeneration requires several critical elements including osteoinduction and osteoconduction buy generic florinef 0.1mg line. Osteoinduction involves the use of growth factors and proteins to cause osteoprogenitor cells to differentiate and stimulate new bone growth. The process of osteocon- duction involves the scaffold that provides the necessary support on which new bone can grow to fill the defect area. As new bone continues to grow to fill the defect area, the process of resorption and remodeling occurs. The development of synthetic materials that can extend the limited supply of natural bone grafts while providing these critical elements has been the focus of much research. One synthetic material that shows promise in this regard is a porous formulation based on the biopolymer poly(propylene glycol-co-fumaric acid) (PPF). This polymer can be crosslinked in the presence of effervescent agents and osteoconductive filler to create a scaffold that mimics the physical and chemical properties of human cancellous bone. A combination of this formulation and an osteoinductive material, such as morselized cancellous autograft, venous blood, or bone marrow, comprises a material with improved handling characteristics and the potential for improved clinical results relative to other composite materials. This paper reviews a series of in vitro and in vivo studies on the use of a PPF-based material as a bone graft extender for use in clinically relevant repair scenarios. AUTOGRAFT BONE Iliac crest autograft is the gold standard for bone graft material. Autograft bone provides the critical elements required for bone growth. The material is also able to maintain the strength and structural integrity of the defect area. Despite these advantages, the material suffers from several disadvantages. The primary disadvantage is the need for a secondary surgical site. Autografts are predominantly removed from the iliac crest of the patient. The procedure of harvesting material from the iliac crest has been shown to cause complications in 4–49% of patients. These complications can range from increased pain—observed in 25% of patients—to infection, sensory loss, and neurologi- cal and vascular injury. Further complications include increased anesthesia time and operative blood loss as well as prolonged recovery time. In addition to the procedural complications, the supply of bone available for harvest is limited. These complications, along with the risk of donor site morbidity and the limited supply of material available for harvest, have pushed the search for alternative materials. ALLOGRAFT BONE Allograft bone is the substitute most often used for autograft bone. It is typically available fresh, frozen, or freeze-dried. This material undergoes extensive processing and donor screening in an effort to reduce the risk of disease transmission. This processing decreases but does not eliminate the risk of disease transmission. In addition, the processing decreases the mechanical and biological properties of the bone, while adding to the cost of the material. In summary, although a viable alternative to autograft bone, allograft bone suffers from concerns of possible disease transmission, recipient rejection, increased cost, and limited availability. SUBSTITUE BONE GRAFT MATERIALS The problems associated with autograft and allograft materials described above, not the least of which is the increasing demand for a limited supply, have acted to fuel the development of substitute materials.