

2018, University of Texas at El Paso, Rune's review: "Chloromycetin generic (Chloramphenicol) 500 mg, 250 mg. Buy online Chloromycetin no RX.".
Some cases disappear in 1 to 2 long-term one with possibilities of reappearance of acne at years but others are persistent and resolve at the age of puberty cheap 500mg chloromycetin visa. Infantile acne purchase 500mg chloromycetin overnight delivery, especially conglobate infantile acne chloromycetin 250 mg with visa, may be related with severe forms of the disease in adoles- Mid-Childhood Acne cence discount 250 mg chloromycetin fast delivery. A family history of severe acne can be present. This type of acne occurs between 1 and 7 years of age. There is one case Acne is very rare in this group and when it occurs should described with elevated levels of LH, follicle-stimulating be evaluated for hyperandrogenemia. Evaluation should be Acne in Infancy and Acne Genetics Dermatology 2003;206:24–28 25 done with a bone age measurement, growth chart and lab- present a statistically significantly earlier menarche (12. They also concluded that the num- hydroxyprogesterone. Occasional reports of acne at this ber of comedones were predictive for the severity of late age because of D-actinomycin are available in the litera- inflammatory acne. This group also showed higher levels of keratosis pilaris of the cheeks and with keratin cysts (mil- DHEAS early in life. A correlation between DHEAS, ia) particularly when they get inflamed. Both lesions are sebum production and free testosterone was found in common in atopics [3, 16]. They evaluated acne versus hormone lev- Prepubertal Acne els at various ages before and after menarche. They were able to conclude that there were no ethnic differences in Increasing number of early onset acne before obvious acne or hormone levels in the groups studied that in- signs of puberty is a recognized phenomenon associated cluded black and white girls. A progressive increase in more with pubertal development than with age. There is number of acne lesions with age and maturation was apparently a genetic predisposition. The most common acne was comedonal; girls with Pubertal development has two components, normal severe acne at the end of the study had more comedones adrenarche related to maturation of adrenal glands and and inflammatory lesions by the age of 10 years and 2. The onset of menarche was also mediated by the hypothalamic-pituitary axis. Early in boys and follow increasing during mid puberty. Exces- development of comedonal acne, DHEAS, free and total sive androgen production may result due to adrenal testosterone were good predictors for severe comedonal hyperandrogenism (exaggerated adrenarche, exuberant acne or a long-term disease. Adverse effects of certain drugs (cortico- lase deficiency, and more rarely androgen producing tu- steroids, anticonvulsants, etc. Ovarian contribution to androgens can be through pubertal hydradenitis suppurative must be considered tumors (malignant and benign), but most commonly due. In more severe cases, especially associated with increase in sebum and urinary excretion in risk of scarring, the use of oral antibiotics and oral iso- of androgenic steroids. A high frequency of acne was tretinoin may be necessary. Resistant, persistent and found in a longitudinal study of adolescent boys, where cases of acne appearing at unusual ages need hormonal the prevalence and severity of acne correlated well with evaluation and proper treatment. Adrenal problems may advanced pubertal maturation. A similar study of the need low doses of oral corticosteroids; polycystic ovarian same authors in early adolescent girls concluded that acne disease can be treated with oral contraceptives that in- can be the first sign of pubertal maturation; significant clude antiandrogens such as cyproterone acetate or the elevations of DHEAS correlated well in girls with come- new low androgenic progestins. Spironolactone can also donal and inflammatory acne.
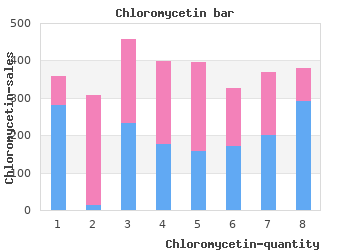
The “mechanical” model of collagen separation causing tendon pain cheap chloromycetin 500mg with amex. Patellar Tendinopathy: Where Does the Pain Come From? Vastus This form of treatment could relieve pain by a medialis number of mechanisms order chloromycetin 250 mg with visa, including denervation purchase 500 mg chloromycetin otc. However purchase chloromycetin 500 mg fast delivery, the proportion of patients who reported Iliotibial skin paresthesia or numbness after patellar ten- band don surgery was the same after arthroscopic or open patellar tenotomy, suggesting a similar degree of denervation in both anterior and poste- rior approaches to the patellar tendon. Nevertheless the procedure is often thera- peutic rather than deleterious. This phenomenon cannot be explained by invoking a purely mechanical model of pain in tendinopathy. The middle third of the patellar tendon is removed in auto- graft ACL reconstruction. Although a great deal of collagen is removed, the patient is generally pain free soon after the operation. Complete Observations about Tendon Pain tendon regeneration takes up to two years, but morphology does not and Imaging Appearances correspond with pain of patellar tendinopathy in those patients who develop it. A variant of the structural model of pain in tendinopathy outlined above argues that it is not torn collagen that hurts per se, but the persisting intact collagen that is placed under greater load Patella because adjacent collagen is injured, and thus becomes painful. Pain is presumed to occur when the proportion of collagen injured reaches a critical threshold and persisting collagen is stressed beyond its normal capacity into a painful overload zone. This model predicts that greater degrees of tendinosis should be more painful than lesser degrees, until complete ten- Patellar don rupture, in which case pain disappears Tibia tendon because there is no longer any collagen left under tension. Data from numerous imaging studies Infrapatellar fat pad argue against this model. In patients with patellar tendon pain, size of collagen abnormality as measured on ultrasound does not correspond with pain, either in cross- sectional studies44,45 or in longitudinal observa- tional studies where change in area of abnormal tissue was monitored. Arthroscopic debridement of the patellar tendon involves mainly excision of the fat pad adhering to the posterior aspect of the This is seen in clinical practice where a patient proximal patellar tendon near its junction with the patella. At surgery, may have a very small, or no, morphological the mucoid degeneration of the posterior portion of the patellar tendon is clearly evident as a cheesy adhesion to the normal tendon. Tissue Impingement Causing Patellar Tendon Pain Both the patellar tendon and the fat pad are in a position where they could be pinched between the patella and the proximal tibia. Could this be the cause of pain in patellar tendinopathy? Impingement as a Mechanism of Patellar Tendon Pain Figure 15. Illustration of the argument for an “impingement” model of pain in patellar tendinopathy. Assuming that the insertion of the Impingement is a form of mechanical load, and patellar tendon to the patella was of a uniform strength, tension on the adds compressive or shearing load to the ten- tendon with the knee flexed should generate more force superficially don’s normal tensile load. Thus, an impingement model was proposed leagues8 argued that tension failure of the whereby pain, and pathology, was caused by the patellar impinging patellar tendon would affect the superficial fibers against the tendon tissue (see text). Thus, they proposed an Furthermore, Johnson’s argument that tension alternative mechanism of the pain and the lesion failure of the patellar tendon would affect the of jumper’s knee: impingement of the inferior superficial fibers more than the deep surface is pole of the patella on the patellar tendon during only valid if the superficial and deep fiber attach- knee flexion (Figure 15. Biomechanical studies, Three clinical observations are inconsistent however, found the superficial attachment to be with deep knee flexion (and impingement) caus- far stronger than the deep. First, pain commences ure can influence the deep fibers preferentially. In in the early phase of landing from a jump, with combination, clinical and research findings sug- quadriceps muscle contraction while the knee is gest that impingement from the patella may not still relatively extended. Second, patients with be a factor in patellar tendinopathy. Third, the superficial portion of the tendon bears too much pain of jumper’s knee does not disappear and of the tensile load while the deep portion of the may actually increase when palpation is per- tendon bears too little of the same load. The angle of the tendon to the patella either with or without quadriceps contrac- Tendon Pain tion was similar in both these groups, suggesting Duri53 speculated that the fat pad has “an impor- that impingement was not a causative factor. However, If one discards the inflammatory model of pain surgical management of the main body of the production, and has reservations about a purely patellar tendon in athletes revealed no macro- mechanical model for the reasons listed above, scopic abnormality of the fat pad.
Short-term hyperventilation to levels of about 25 mm Hg can be lifesaving in the patient with impending herniation generic chloromycetin 500 mg with mastercard. Subdural and epidural hematomas should be evacu- ated promptly when associated with a significant mass effect purchase chloromycetin 500mg with amex, because it has been shown that there is a significant poorer outcome with surgical delays of greater than 4 hours cheap chloromycetin 250 mg amex. The literature supports a standard recommendation that corticosteroids should not be used for neuroprotection or control of ICP in patients with severe TBI chloromycetin 250mg otc. A 22-year-old man is transferred to your hospital from a local hospital, where he presented 3 hours ago with closed head trauma. At the first hospital where he was taken, he was given pain medications, and a CT scan was performed; the CT scan was negative. The patient is awake and complains only of moderate headache. The fam- ily is concerned about the development of seizures in the future, because they had a relative who had that problem. What would you recommend regarding prophylaxis for seizures in this patient? Phenytoin for 1 to 2 weeks B Carbamazepine for 6 months C. Obtain an electroencephalogram; if it is abnormal, start phenytoin D. Do not start any antiseizure medication at this time Key Concept/Objective: To understand the evaluation of the risk of posttraumatic epilepsy The risk of epilepsy in patients with closed-head injury is relatively small: 2% to 5% in all patients and about 10% to 20% in patients with severe closed-head injury. A higher inci- dence of seizures has been seen in patients with depressed skull fractures (15%), hematomas (31%), and penetrating brain wounds (50%). This patient has a mild, closed injury, and he is at very low risk for developing seizures. Because most patients who devel- op posttraumatic epilepsy in the first week after injury will have recurrent seizures for some time, anticonvulsant therapy is indicated in documented cases. Controlled, ran- domized studies have shown that the use of phenytoin, phenobarbital, carbamazepine, and valproate do not prevent the development of posttraumatic epilepsy beyond the first week after injury. It is recommended as a standard of care that these medications should not be used to prevent posttraumatic epilepsy in patients who have not had a seizure. A 44-year-old woman presents to your clinic complaining of persistent problems since being in a car acci- dent 2 years ago. At the time of the accident she suffered moderate head trauma, which required admis- sion to a hospital for 3 days. Since then, she has felt as if she is not the same person. She has had prob- 16 BOARD REVIEW lems with her husband, and she feels sad all the time. She also has lost interest in social activities, and she has lost 12 lb. What is the most likely diagnosis, and how would you treat this patient’s symptoms? The patient probably has a personality disorder; she should not have sequelae from accidents of this nature; refer for psychotherapy B. The patient probably has an undisclosed substance abuse problem; refer to psychiatry C. The patient probably has neuropsychiatric sequelae from the accident; educate her about the possible sequelae, and start a selective serotonin reuptake inhibitor (SSRI) for depression D. The patient probably has major depression, but it is unlikely that this depression is related to the accident; start an SSRI Key Concept/Objective: To understand neuropsychiatric sequelae of head trauma The neuropsychiatric sequelae of brain injury, both socially and in the workplace, are well appreciated. Neurologic abnormalities may not be as distressing to the patient or the patient’s family as personality changes and inappropriate behavior. Suitable treatment of neurobehavioral sequelae will often decrease patient and caregiver distress and markedly improve overall outcome. The SSRIs are favored because they are safe and easy to admin- ister. Other common neuropsychiatric sequelae are irritability, aggression, attention deficits, seizures, memory problems, and posttraumatic stress disorder.